Neuroblog
Editor Myself: Neuroblog on neurology, clinical neurophysiology etc.
3.21.2005
Minimally Conscious State
The Aspen workgroup defined the minimally conscious state (MCS) as a condition of severely altered consciousness in which the person demonstrates minimal but definite behavioral evidence of self or environmental awareness (Giacino et al, 1997).
As with patients in the vegetative state (VS), patients in MCS have spontaneous eye opening and sleep-wake cycles. Arousal may range from obtundation to full wakefulness but most patients in MCS will have periods of normal arousal. (Table 2 summarizes the clinical features of coma, VS and MCS [Giacino et al, 1997].)
Table : Comparison of clinical features of coma, VS and MCS (Giacino et al, 1997)
Arousal Awareness Consciousness
Coma
Eyes do not open spontaneously or in response to stimulation
No evidence of perception, consciousness ability, or purposeful motor activity (e.g. command following)
No evidence of yes/no responses, verbalization, or gesture
VS
Eyes open spontaneously; sleep-wake cycle resumes; arousal often sluggish, poorly sustained but may be normal
No evidence of perception, consciousness ability, or purposeful motor activity
No evidence of yes/no responses, verbalization, or gesture
MCS
Eyes open spontaneously; sleep-wake cycles; arousal level ranges from obtunded to normal
Reproducible but inconsistent evidence of perception, consciousness ability, or purposeful motor activity; visual tracking often intact
Ranges from none to unreliable and inconsistent yes/no responses, verbalization and gesture
Methods of evaluation in the diagnosis of MCS
There are no standard evaluation procedures for the neurological examination of patients with minimal
consciousness. Most neurologists are familiar with the clinical examination of the patient with impaired
consciousness. Nevertheless, frequent errors in diagnosis occur (Childs et al, 1993; Andrews et al, 1996) either because of a misinterpretation in results or examinations that are inadequate to detect minimal, inconsistent responsiveness.
The general goals of the neurological examination of patients with impaired
consciousness include assessment of the integrity of brainstem pathways (e.g. pupilary responses, ocular movements, oculovestibular reflexes, breathing patterns) and the presence of higher level cortical functions (e.g. purposeful, voluntary behaviors). It is the latter that determines the distinction of MCS from VS or higher level states. Patients who fit the definition of MCS must have some restoration of cortical functioning and it is the job of the examiner to
systematically elicit and distinguish behaviors that are evidence of cortical activity.
A
systematic approach to the examination of patients with impaired
consciousness includes the following steps:
Brainstem integrity and other subcortical evaluation
Pupillary response, blink reflex to visual threat
Ocular movements, gaze deviations
Oculovestibular reflexes (occulocephalic maneuvers, calorics)
Corneal response
Gag reflex
Breathing pattern
Decerebrate postures
Other posturing, reflexes and tone
Cortical functioning
observation of spontaneous activity
purposeful, complex movements (involving cortically mediated isolated motor control) vs. posturing (decorticate or decerebrate) or reflex or stereotyped, patterned (subcortically mediated) movements (Note: Pilon and Sullivan (1996) observed differing postural profiles for VS and MCS patients. VS patients demonstrated classic decerebrate, decorticate or hypotonic postures, whereas MCS patients either symmetric, asymmetric or global flexion postures. However, no other pattern of reflex responses discriminated the 2 groups.)
spontaneous vocalizations or verbalizations
eye movements (signs of fixation or tracking vs. nonspecific roving or no movement)
responses to stimulation or environment
tracking or fixation to stimuli (try
salient stimuli such as familiar pictures, faces, money, mirror)
verbal stimulation (e.g. patient's name, commands, social greetings):
Begin with simple commands sampling a variety of areas under different neural control, favoring those areas of potentially preserved movement.
eye commands--e.g. 'look up', 'blink twice';
limb commands--e.g. 'make a fist', 'show 2 fingers', 'raise your arm';
oral commands--e.g. 'open mouth,' 'stick out tongue';
axial or whole body commands--e.g. 'turn your head,' 'lean forward').
ask patient to 'stop moving' or 'hold still' to distinguish from spontaneous repetitive movements.
noxious stimulation
look for localization or purposeful defensive maneuvers vs. reflexive or generalized, stereotyped movements or facial
expressions.
responses in contingent relationship to environment or other stimuli
look for intentional reach for or manipulation of objects on or around the patient (e.g. pulling at tubes, clothing, items placed in the hand)
look for changes in facial
expression contingent on stimuli such as familiar voices, particular conversation, pictures,
music, etc.
look for attempts at purposeful mobility in bed, chair, and even ambulation
gestural behaviors indicating intentive
communication (e.g. yes/no signals)
D. Pitfalls in the diagnosis of MCS and examination strategies to enhance detection of
consciousnessThere are several "pitfalls" in distinguishing MCS from VS. These include:
attributing purposeful intent for stimulus contingency to reflexive or generalized responses
inadequate evaluation to detect conscious behavior--e.g. too brief a sampling
time, inadequate arousal, insufficient choice of stimuli
over or underconsideration of family or other's observation of purposeful behavior (recognize that family may be first to observe signs of
consciousness and also may tend to overattribute purposefulness to a patient's responses)
simple, cortically mediated behaviors of uncertain cognitive significance--e.g. tracking, simple isolated limb movements
confounding factors affecting arousal
The evaluation of patients with impaired
consciousness may be confounded by a number of factors. These include effects of centrally acting medications, concurrent illness, distracting environmental stimuli, the patient's state of arousal at the
time of evaluation and the frequent occurrence of uninhibited reflex or other stereotypical responses,. The examiner should use strategies to account for some of these confounds and maximize the chance of detecting signs of conscious behavior. Strategies include:
E. Standardized assessment tools and scales
1. Scales for impaired
consciousnessAside from the clinical bedside examination, there are a number of more objective, standardized assessment tools and scales to track patients transitioning between unconsciousness and
consciousness. The Glasgow Coma Scale (GCS) (Teasdale and Jennett, 1974) is the most commonly used
instrument. The Disability Rating Scale (Rappaport et al, 1982) is frequently used in rehabilitation populations but basically incorporates the same criteria as the GCS for impaired
consciousness. The Rancho Los Amigos Levels of Cognitive Functioning (RLA) (Hagen, 1972) is also commonly used in rehabilitation populations, especially for patients with traumatic
brain injury (table 4). The first three levels of this 8 level scale describe patients in coma (RLA I--no response), vegetative state (RLA II--generalized responses) and the transition between vegetative and minimally conscious states (RLA III--localized responses). Another similar scale, used to describe stages of recovery after diffuse
brain injury, incorporates some of the more familiar neurological nomenclature (table 5) (Katz, 1993, 1997, Katz and Alexander, 1994; Alexander, 1982).
Table 4: Rancho Los Amigos Levels of Cognitive Functioning (Hagen et al, 1972)
I. No Response
II. Generalized Responses
III. Localized Responses
IV. Confused - Agitated
V. Confused - Inappropriate
VI. Confused - Appropriate
VII. Automatic - Appropriate
VIII. Purposeful and Appropriate
Table 5: Stages of Recovery from Diffuse Traumatic
Brain Injury (Katz, 1993, 1997, Katz and Alexander, 1994; Alexander, 1982)
1.Coma: unresponsive, eyes closed
2.Vegetative state / wakeful unconsciousness: no cognitive responsiveness, gross wakefulness, sleep-wake cycles
3. Minimally conscious state: purposeful wakefulness, responds to some commands, often mute
4.Confusional state: recovered speech, amnesic (PTA), severe attentional deficits, agitated, hypoaroused or labile behavior
5.Post-confusional / evolving independence: resolution PTA, cognitive improvement, achieving independence in daily self care, improving social interaction; developing independence at home
6.Social competence / community reentry: recovering cognitive abilities, goal directed behaviors, social skills, personality; developing independence in community; returning to academic or vocational pursuits
2. Assessment protocols for impaired
consciousnessNone of the above mentioned scales are sensitive to small changes in responsiveness in unconscious and minimally conscious patients. Several
instruments have been developed for this purpose, including the Western Neuro Sensory Stimulation Profile (Ansell et al, 1989), the Coma Recovery Scale (Giacino et al, 1991), the Sensory Stimulation Assessment Measure (Rader & Ellis, 1994) and the Coma/Near Coma Scale (Rappaport et al., 1992). These scales provide a
systematic measure of responses using a standardized stimulation protocol. Distinctions between VS and MCS can be made using these scales based on total scores or subscores on individual items demonstrating purposeful responses. Evaluation of these scales on the same group of patients demonstrated fairly high correlations between them (mild floor effect on the Western Neuro Profile) and some prognostic value (O'
Dell et al 1996).
3. Quantitative assessment of impaired
consciousnessWhyte and colleagues (1995) developed a quantitative method of assessing
consciousness in minimally responsive patients. These procedures are an attempt to remove subjective judgement and substitute statistically-based, single subject design trials to assess whether responses are consciously mediated. For instance, patients may be presented either a photograph or white card or both in the left or right visual field in random
order. The patients responses are recorded as looking left, right or neither direction in response to stimuli. Statistical evaluation is carried out to determine whether gaze was purposefully directed toward the more
salient stimulus greater than chance. This method might also detect a visual field deficit or unilateral neglect in patients with impaired
consciousness. Similar quantitative procedures can be carried out for command following and yes/ no responsiveness (DiPasquale & Whyte, 1996).
IV. Prognosis
A. Outcome of MCS
There is very little specific
information about the prognosis of the MCS. Rappaport and coworkers (1992) reported improvement in 25% of a small group of patients with impaired
consciousness followed over a 4-month period. Only those in MCS (referred to as "near-coma") improved; none in VS improved in the follow-up period.
There is to date only one
systematic study comparing outcome of patients in VS versus MCS (Giacino & Kalmar, 1997). In this study 55 patients in VS were compared to 49 patients in MCS when they were first evaluated an average of 9.6 weeks post-injury. Causes of injury were traumatic (n=70) and non-traumatic (n=34) (mostly anoxic
brain injury and stroke). Using the Disability Rating Scale as the outcome measure at 1,3,6 and 12 months post-injury they reported the following findings:
Patients initially in MCS fared better than those initially in VS, the differences becoming
progressively more apparent at 3, 6 and 12 months post-injury.
Patients in MCS after traumatic
brain injury had less disability than after non-traumatic injuries. (There were no significant differences in outcome between traumatic and non-traumatic causes among patients initially in VS.)
The probability of a more favorable outcome (moderate or no disability) by one year was much greater for the MCS group (38%) than the VS group (2%) and only occurred in those patients with traumatic
brain injury.
43% of the MCS group remained severely disabled or worse (1/10 of the non-traumatic MCS group was vegetative and 2/10 died) at 12 months.
So-called "borderzone" clinical signs--visual tracking, motor agitation--were much more prevalent among patients in MCS than those in VS. 73% of patients in VS who displayed tracking recovered
consciousness, whereas 45% without tracking recovered
consciousness.
B. MCS and VS in the natural
history of recovery of
brain injury
MCS and VS should be viewed as a part of the natural
history of diffuse and multifocal
brain injury. The majority of patients with diffuse
brain injury (traumatic and non-traumatic) pass through a series of stages that are qualitatively similar across a wide range of severity (table 5). The duration of these stages and severity of impairments vary in proportion to injury severity (Katz, 1997; Katz & Alexander, 1994). Most patients with
brain injury severe enough to cause unconsciousness, probably
progress through stages of unconsciousness, with eyes closed (coma), to unconsciousness with eyes open (vegetative state), to a stage of inconsistent, erratic responsiveness (minimally conscious state). Once
consciousness is clearly established, patients enter a stage of impaired attention and anterograde amnesia (e.g. post-traumatic amnesia) (confusional state) followed by a post-confusion phase of recovery.
In patients with very severe damage, recovery may stall at one or another stage (e.g. "permanent" vegetative state or minimally conscious state). Patients with less severe injuries may transition through the early stages quickly and discreet stages may not be clinically apparent. It remains to be established what proportion of patients recovering from unconsciousness at different severities of injury evolve through discernible coma, VS and MCS stages.
Viewed in this way, the transition from unconsciousness to
consciousness is a continuum without distinct boundaries. As the transition
progresses, and cortical function resumes, the consistency and
complexity of behavior increases. The first signs of the transition may be an increase in alertness and spontaneous movement with lower levels of stimulation, such as the arrival of the examiner (Wilson et al., 1996). At the borderzone, behaviors such as tracking,
emotional
expressions and non-stereotyped motor sequences resume heralding higher level cognitive behaviors (Andrews, 1993; Ansell, 1995; Multisociety Task Force on PVS, 1994; Giacino & Kalmar, 1997). A small number of patients will recover these "borderzone" behaviors without resuming any other cognitive behavior, such as following commands (Andrews, 1993; Giacino & Kalmar, 1997).
V. Treatment implications
Decisions regarding
basic medical and rehabilitative care of patients in VS and MCS are largely the same. Some treatment decisions may differ, however, based on 3 factors: 1. Differences in prognosis; 2. Potential for establishing
communication; 3. Possibility of pain and suffering.
The more favorable prognosis of MCS over VS and the absence of established guidelines for permanence of MCS would affect decisions with respect to duration of rehabilitative efforts and withdrawal of treatment, including fluid and nutrition. The potential for
communication supports greater emphasis on strategies to promote arousal and developing alternative or augmentative
systems of
communication. The potential for pain and suffering in patients in MCS, in contrast to patients in VS, supports a greater emphasis on comfort measures and on administering or withholding treatment that might cause or avoid discomfort.
11.24.2004
Medical Informatics in Neurology
Authored by Hamid Sami, MD, MSc, Clinical Neurophysiology/Neuromuscular Fellow, Department of Neurology, Yale University School of Medicine
Hamid Sami, MD, MSc, is a member of the following medical societies: American Academy of Neurology, American Association of Electrodiagnostic Medicine, American Medical Association, and American Medical Informatics Association
WHAT IS MEDICAL INFORMATICS?
Medical informatics is most simply defined as computer applications in medical care. The definition can be more complicated. Biomedical informatics is an emerging discipline that has been defined as the study, invention, and implementation of structures and algorithms to improve communication, understanding, and management of medical information. The end objective of biomedical informatics is the integration of data, knowledge, and tools necessary to apply that data and knowledge in the decision-making process associated with patient care. The focus on the structures and algorithms necessary to manipulate the information separates biomedical informatics from other medical disciplines where information content is the focus.
According to Van Bemmel, medical informatics comprises the theoretical and practical aspects of information processing and communication based on knowledge and experience derived from processes in medicine and health care.
The applications of computers in health care are very extensive, but the field of medical informatics can be structured or divided into the following domains:
Signal processing - ECG, electroencephalography (EEG), electromyography (EMG) analysis by computer
Image processing - Radiography, US, CT scanning, MRI/magnetic resonance angiography (MRA), single photon emission computed tomography (SPECT) scanning/positron emission tomography (PET) scanning, cerebral angiography
Computerized patient records
Decision support systems
Telemedicine
Internet and web-based medical communications
SIGNAL PROCESSING (EEG, EMG, ECG)
Computers are useful devices for processing electrical signals from various sources, such as ECG for detection of heart dysrhythmias and EEG for analysis and detection of spike and sharp waves that can sometimes be missed by the neurologist. The caveat is that many of these systems have a high rate of false-positive results for detection of sharp waves or other epileptiform discharges that may not be relevant to the clinical situation. As for any automated system, for routine clinical application, computerized EEG evaluation needs analysis by an experienced epileptologist.
In nerve conduction studies and EMG, signal processing with computers can aid in waveform analysis, compound muscle action potentials (CMAP) and sensory nerve action potentials (SNAP) measurements, and amplitude and area quantitative measurements. Combined with a comparison system for reference range values, a custom-made report can be produced for easy recognition of abnormal values and final diagnosis. In general, computerized EMG can help the less experienced neurologist or electromyographer with early diagnosis of subtle EMG changes.
IMAGE PROCESSING (RADIOGRAPHY, US, CT SCANNING, MRI/MRA, SPECT/PET, CEREBRAL ANG
Image processing and pattern recognition are important fields in medical informatics, specifically in neuroinformatics as an emerging domain for CT scanning, MRI of the brain, and other new techniques such as SPECT, PET, and functional MRI (fMRI). For example, processing of spatially distributed patterns of brain activation in fMRI data sets using computerized analysis helps determine pathophysiology of many neurologic disorders and define functional structures of the brain.
COMPUTERIZED PATIENT RECORDS
In the new millennium, information technology will catalyze dramatic change in many aspects of medicine, including patient records. Good medical care requires accurate records of greater detail than in the past. Malpractice protection mandates more organized and complete records. Third party payers are requiring more justification for the expenses generated by physicians’ actions. Today’s economics require more efficient and cost-effective methods of keeping the patient’s clinical records. In 1991, the Institute of Medicine (IOM) released an influential report, The Computer-Based Patient Record: An Essential Technology for Health Care. The report advocated adoption of the computer-based patient record (CPR) as standard medical practice.
According to the report, “CPRs and CPR systems can respond to health care’s need for a ‘central nervous system’ to manage the complexities of modern medicine – from patient care to public health to health care policy.” The report described the CPR as a continuous chronological history of a patient’s medical care linked to various aids for their user, such as programmed reminders and alerts generated by decision-making systems. The IOM report led to the creation of the Computer-Based Patient Record Institute, an advocacy group that is supported by corporations in the health care, insurance, data-processing, and computer industries, as well as by some professional groups.
Definition of CPR
A CPR is electronically maintained information about an individual’s lifetime health status and health care. CPRs are not merely automated forms of today’s paper-based medical records but are the first steps toward integrating patient information into the entire scope of health information in all media forms. CPR systems facilitate the capture, storage, processing, communication, security, and presentation of nonredundant health information. CPR systems provide availability of complete and accurate patient data, clinical reminders and alerts, decision support, and links to bodies of related data and knowledge bases. CPR systems can warn a caregiver when the patient has an allergy to a medication being prescribed, can provide the latest research on treatment modalities, and can organize volumes of information about a patient’s chronic condition.
Use of CPR
Despite more than two decades of research, use of CPRs by physicians is not widespread. In the past 20 years, several systems for the electronic storage of patient data have been developed and used in clinical settings. Early developments involved tasks such as administration, billing, and planning. The early versions of the CPR included categories of patient data that were relatively easy to represent in a structured fashion, such as laboratory data, discharge diagnosis, and medications. The advantages of structured data are obvious: data can be presented in different views and formats, thereby eliminating the need for redundancy. However, the computerized collection of structured progress notes, directly from physicians, was long thought to be unattainable goal. Currently, fewer than 10% of US physicians use a CPR, but enthusiasm for its use is growing. Among primary care physicians, use of CPRs is gaining popularity.
However, usage figures are very low and disappointing with respect to specialists. Several reasons may account for this. Most primary care physicians run a private or small group practice. In contrast, hospital-based specialists work in large institutions in a more complex setting, involving a much larger number of departments and personnel. Therefore, the use of CPR systems has much logistic and financial impact, and stand-alone systems often introduce extra work because they may at best augment, but do not replace, the paper record. Furthermore, because specialists have different medical domains, CPRs should be tailored to their specific needs. Finally, in contrast to primary care physicians, specialists often keep more extensive records, making data entry more time consuming.
Despite these complicating factors, there are many benefits to the use of CPRs in specialized care. Access to multiple sources of patient data, including signals and images, and sharing of patient records can provide a more complete knowledge of the patient and improve the continuity of care.
CPRs or electronic health records (EHRs) are and will be a very important part of medical practice. Recently announced was "The Decade of Health Information Technology," which emphasizes always-current, always-available EHRs for patients. EHRs can improve quality of care, reduce medical errors, and lower administrative costs. Electronic record-keeping has the potential to produce savings of 10% of annual spending on health care, while improving care for patients and providing new support for health care professionals. At the same time, the security and privacy of electronic medical records would be improved compared to paper-based records.
Many systems are available and require standardization for ease of use among physician; many clinicians may need further computer training, so available systems should be designed to decrease administrative work for physicians and enhance the physician-patient relationship.
The IOM has identified a set of 8 core functions that an electronic medical records software system should have:
Health information and patient data
Laboratory results management
Computerized order management
Decision support system
Electronic communication and connectivity
Patient support and education
Administrative processes
Reporting
Additionally, the following functionalities help better adoption of the CPR by physicians:
Transition or flexibility in moving from desktop to handheld computing devices
Structured data entry to accommodate the diversity of specialized care
Options to express findings and conclusions in free text or definition of normal
Graphical data entry for body maps and radiology images
Automatization and improvement of transcription and upload process
Enhancement of faxback service and upgrade to electronic file transfer or Web access service
Enhancement of decision support systems and implementation of artificial intelligence such as drug interaction service and various clinical guidelines
DECISION SUPPORT SYSTEMS
Decision support systems are real-time computerized algorithms that help physicians in their clinical practice. For example, when clinicians perform a task (eg, order entry) using the CPR, they are warned if the task appears to be inappropriate on the basis of patient data. The system presents this warning automatically using consensus-based clinical decision support "rules" that are derived from medical knowledge (or financial data) and patient-specific information.
For example, EMG expert systems such as EMG Assistant can help electromyographers through a sophisticated analysis of the input data and provide them with the most likely diagnosis that objectively best explains the findings. These programs can help doctors understand the readings as they develop the field experience to analyze the data themselves.
TELEMEDICINE
Telemedicine is distance consultation among health professionals or between health professionals and patients by use of telecommunications technology such as real-time audio or visual systems, most notably video conferencing. The potential advantages are obvious in dispersed communities, where expertise is thinly spread, and when traveling is difficult or inconvenient for doctor or patient. Uses are wide and varied and include direct interview and history taking, observation of physical signs, and distance reporting of imaging procedures. The location of consultation varies from hospital inpatient and outpatient settings, to broader residential and home settings, and even outer space.
Some hospitals in the United States are using broadband technology to improve patient care and cope with a national shortage of physicians in certain specialties. For example, in one hospital in California, patients in the intensive care unit (ICU) are being monitored by doctors a mile away in a control room called the eICU.
Prescription improvement packages offer physicians a wireless handheld electronic prescribing unit, a wireless access point, and a 1-year subscription to an e-prescribing service. This allows physicians to discard their prescription pads in favor of electronic transmissions to any pharmacy. A recent report by the Foundation for eHealth Initiative estimates that nationwide implementation of e-prescribing could save the US health care system $29 billion a year.
With advancing communications protocols, neurologists can view their patients’ radiology images and diagnose their diseases from remote locations. Even computer-assisted neurosurgery is possible. Another convenient and cost-effective use of telemedicine will be in teaching and consulting situations, especially when large distances separate educator and learner. In areas of the country where patients are long distances from a medical center or when transportation is a problem, such systems will be very helpful.
Telemedicine will not be easily accepted by physicians as a routine substitute for direct patient care because it lacks the intimacy of face-to-face conversations, but it is an exciting and beneficial addition to the world of healthcare. More of it will undoubtedly be available in the near future.
Remember that communicating with patients through email is prudent only if the following guidelines are employed:
Establish turnaround time for messages and do not use email for urgent matters.
Inform patients about privacy issues.
Establish types of transactions (eg, prescription refill, appointment scheduling) and sensitivity of subject matter (eg, HIV status, mental health care) permitted over email.
Instruct patients to put the category of transaction (eg, prescription, appointment, medical advice, billing question) in the subject line of the email message for filtering.
Request that patients put their name and patient identification number in the body of the message.
Configure automatic reply to acknowledge receipt of messages.
Print all messages, with replies and confirmation of receipt, and place in patient`s paper chart.
Send a new message to inform patient of completion of request.
Request that patients use autoreply feature to acknowledge reading provider`s message.
Maintain a mailing list of patients but do not send group mailings where recipients are visible to each other. Use the blind courtesy copy feature in email software.
Avoid anger, sarcasm, harsh criticism, and libelous references to third parties in messages.
Consider obtaining patient`s informed consent for use of email.
Never forward patient-identifiable information to a third party without the patient`s express permission.
Use encryption for all messages when encryption technology becomes widely available, user-friendly, and practical.
Do not use unencrypted wireless communications with patient-identifiable information.
Commit policy decisions to writing and electronic form.
INTERNET AND WEB-BASED MEDICAL COMMUNICATION
Despite the tremendous growth of the Internet and the vast amount of information available to medical practitioners, busy physicians (especially those in clinical practice) have little time to spend exploring the Internet. In some cases, physicians simply do not know how to access required medical information in the best and fastest possible way. Many physicians do not know how beneficial the Internet can be for their medical careers, especially in such areas as patient care, academic work, or research.
The Internet has attracted considerable attention as a means to improve health and health care delivery, but how prevalent Internet use is in health care or what impact it has on health care utilization is not clear. Available estimates of use and impact vary widely. Approximately 40% of respondents with Internet access reported using the Internet to look for advice or information about health or health care in 2001. Six percent reported using email to contact a physician or other health care professional. About one third of those using the Internet for health reported that using the Internet affected a decision about health or their health care, but very few reported impacts on measurable health care utilization, 94% said that Internet use had no effect on the number of physician visits they had, and 93% said it had no effect on the number of telephone contacts. Five percent or less reported use of the Internet to obtain prescriptions or purchase pharmaceutical products.
An increasing proportion of the public is using the Internet for health information. This is expected to have a profound effect on medicine, but whether this effect will be beneficial or harmful is unclear. The advantages of the Internet as a source of health information include convenient access to a massive volume of information, ease of updating information, and the potential for interactive formats that promote understanding and retention of information. Health information on the Internet may make patients better informed, leading to better health outcomes, more appropriate use of health service resources, and a stronger physician-patient relationship. However, health information on the Internet may be misleading or misinterpreted, compromising health behaviors and health outcomes or resulting in inappropriate requests for clinical interventions. Physicians may accede to inappropriate requests, either because refusal is time consuming or because they fear refusal would weaken the physician-patientrelationship. Responding to inappropriate patient requests may be particularly difficult in managed care, where patients may believe that physician refusals may be motivated by the need to control costs.
More-informed patients often have a more favorable prognosis, and doctors can help make patients better informed by supplying reliable Internet sites. Researchers at University of Iowa tested the benefits of an "Internet prescription," or a list of Web addresses containing information relevant to patients' medical conditions. In the study, patients and their families that received such information were more likely to use the Internet to find health information than patients who were not. One of every 3 parents receiving Internet prescriptions for their child’s health said they used it. Also, 66% of the health-related Web sites used by parents in the prescription group were sites recommended by the physicians.
In conclusion, the Internet and Web has had important impact in the practice of medicine. Physicians need to know the importance of this media and how to use it in a pragmatic and efficient way. Many physicians believe that they save personal time by using the Internet and that they can use the Internet for better practice of medicine. They can have easy access to clinical guidelines, journal contents, and reference textbooks and even provide patients with educational materials. Physicians will be able to obtain information on state-of-the-art conferences and have direct communication with other physicians and specialists or practice telemedicine, thereby expanding the depth and extent of medical knowledge and providing better diagnosis and patient care.
TEST QUESTIONS
CME Question 1: There are different domains of medical informatics. Which of the following is not a medical informatics specialty?
A: Signal and image processing B: Computerized patient records C: Decision support systems D: Computer programming and information security E: Telemedicine and Web-based medical communication The correct answer is D: Computer programming and security, although very important in medical informatics, are not a medical informatics field of work or research. Programming and security are better conducted by computer programmers and security experts. Medical informatics specialists should provide their inputs and recommendations for designing practical solutions for better practice of medicine.
CME Question 2: What are the advantages of using computerized patient records?
A: No scattering of medical information, increased availability and accessibility of patient records B: More organized and complete records for malpractice protection C: More justification for the expenses generated by physicians' actions D: Ability to search for relevant patient information and research E: All of the above The correct answer is E: Computerized patient records are necessary tools for effective medical care today because of the above-mentioned reasons. A computerized patient record is electronically maintained information about an individual’s lifetime health status and health care. Computerized records facilitate the capture, storage, processing, communication, security, and presentation of nonredundant health information.
Pearl Question 1 (T/F): Electroencephalography (EEG) analysis by computer can be used by all physicians to diagnose seizure disorders.
The correct answer is False: Although EEG analysis by computer is very good for detection of spike and sharp waves, it has a very high rate of false-positive results and always requires analysis by an experienced neurologist.
Pearl Question 2 (T/F): Electromyography (EMG) analysis with computers can aid in early diagnosis of subtle EMG changes.
The correct answer is True: In nerve conduction studies and EMG, signal processing with computers can help in waveform analysis, compound muscle action potentials (CMAP) and sensory nerve action potentials (SNAP) measurements, and amplitude and area quantitative measurements and can be an excellent tool for better recognition or early diagnosis of neuromuscular disorders.
Pearl Question 3 (T/F): Physicians and patients may communicate through email.
The correct answer is False: Communicating with patients through email is prudent only if the following guidelines are employed:
Establish turnaround time for messages and do not use email for urgent matters.
Inform patients about privacy issues.
Establish types of transactions (eg, prescription refill, appointment scheduling) and sensitivity of subject matter (eg, HIV status, mental health care) permitted over email.
Instruct patients to put the category of transaction (eg, prescription, appointment, medical advice, billing question) in the subject line of the email message for filtering.
Request that patients put their name and patient identification number in the body of the message.
Configure automatic reply to acknowledge receipt of messages.
Print all messages, with replies and confirmation of receipt, and place in patient`s paper chart.
Send a new message to inform patient of completion of request.
Request that patients use autoreply feature to acknowledge reading provider`s message.
Maintain a mailing list of patients but do not send group mailings where recipients are visible to each other. Use the blind courtesy copy feature in email software.
Avoid anger, sarcasm, harsh criticism, and libelous references to third parties in messages.
Consider obtaining patient`s informed consent for use of email.
Never forward patient-identifiable information to a third party without the patient`s express permission.
Use encryption for all messages when encryption technology becomes widely available, user-friendly, and practical.
Do not use unencrypted wireless communications with patient-identifiable information.
Commit policy decisions to writing and electronic form.
Pearl Question 4 (T/F): Telemedicine can replace physician-patient relationships.
The correct answer is False: Although telemedicine has many potential advantages, especially in certain specialties such as dermatology, and can reduce patient care costs, it cannot and should not replace direct physician-patient relationships whenever possible.
BIBLIOGRAPHY
Brown SW: Will teleneurology hit the big time?. Lancet Neurol 2004 Sep; 3(9): 517-8[Medline].
Feistner H, Munte TF, Strempel J, Heinze HJ: Computer-aided EMG-analysis in patients with neurogenic lesions. Electromyogr Clin Neurophysiol 1992; 32(9): 463-9[Medline].
Hinrichs H, Feistner H, Awiszus F, et al: Use of automatic, computer-assisted EEG analysis in clinical practice. Fortschr Neurol Psychiatr 1997; 65(8): 354-60[Medline].
ONCHIT: Health Information Technology Strategic Framework Report. Available at: http://www.hhs.gov/onchit/framework/hitframework.pdf. Office of National Coordinator for Health Information Technology; 2004[Full Text].
Shams OE, Jabre JF: EMG: Your guide to putting it into practice. Practical Neurology 2004; 3(7): 55-59.
Van Bemmel JH, Musen MA: What is Medical Informatics?. Available at: http://www.mihandbook.stanford.edu/handbook/home.htm. Handbook of Medical Informatics. Vol 1. 1999[Full Text].
van Bemmel JH: The structure of medical informatics. Med Inform (Lond) 1984 Jul-Dec; 9(3-4): 175-80[Medline].
8.01.2004
Drugs That May Cause Neuropathy or Are Neurotxic for Patient With Neuropathy
7.31.2004
Barriers to Management of Patients with Surgically Remediable Intractable Epilepsy
Between 400,000 and 600,000 people in the United States have medically intractable seizures. Of these, it is estimated that between 100,000 and 200,000 patients with intractable epilepsy are eligible for surgery. Despite this, only 2,000-3,000 surgical procedures are performed annually in the US. The reason for the disparity between the potential number of surgical procedures that could be performed and the actual number performed is the focus of this review. Although the literature is replete with information on the barriers to patient access to health care in general, there is limited information specifically on the barriers to patients receiving surgical treatment for surgically remediable intractable epilepsy. Where possible, direct evidence regarding the surgical treatment of epilepsy will be presented. If this evidence is lacking for critical topics, indirect evidence regarding barriers to accessing general surgical procedures or general healthcare services will be presented.
BARRIERS TO THE SURGICAL TREATMENT OF SURGICALLY REMEDIABLE INTRACTABLE EPILEPSY
Patients with Intractable Epilepsy are Severely Disabled
Patients with intractable epilepsy are sometimes severely disabled and disability can create barriers to receiving recommended care. Patients with intractable epilepsy often have difficulty arranging transportation to healthcare appointments because they cannot drive and are dependent on family members or public transportation. he inability to hold a driver's license was the most frequently cited restriction that epilepsy had placed on patient's lifestyles. Patients often struggle with employment problems. The probability of employment for individuals with epilepsy is reduced by 47% in men and 41% in women. Patients feel epilepsy carries a stigma that fuels discrimination and causes isolation. In one study, 46% of patients felt they suffered discrimination at work. In another study, the few patients who were employed reported that it was difficult to take time off from work for healthcare appointments or participation in epilepsy research because they had used all of their sick leave.
Seizure activity, depression, and inability to remember dates, times, and interactions results in patients not returning phone calls, missing appointments, and struggling with the basic skills necessary to maintain their health.3 Patients often attribute their disability to medication side effects.3,4 In an United Kingdom study, 56% of patients with epilepsy reported current medication side effects despite the fact that 58% of this sample of patients had not had an epilepsy attack in the previous year.

7.01.2004
Patient Assistance Programs
Brand Name List
NeedyMeds
6.29.2004
Paraneoplastic syndromes
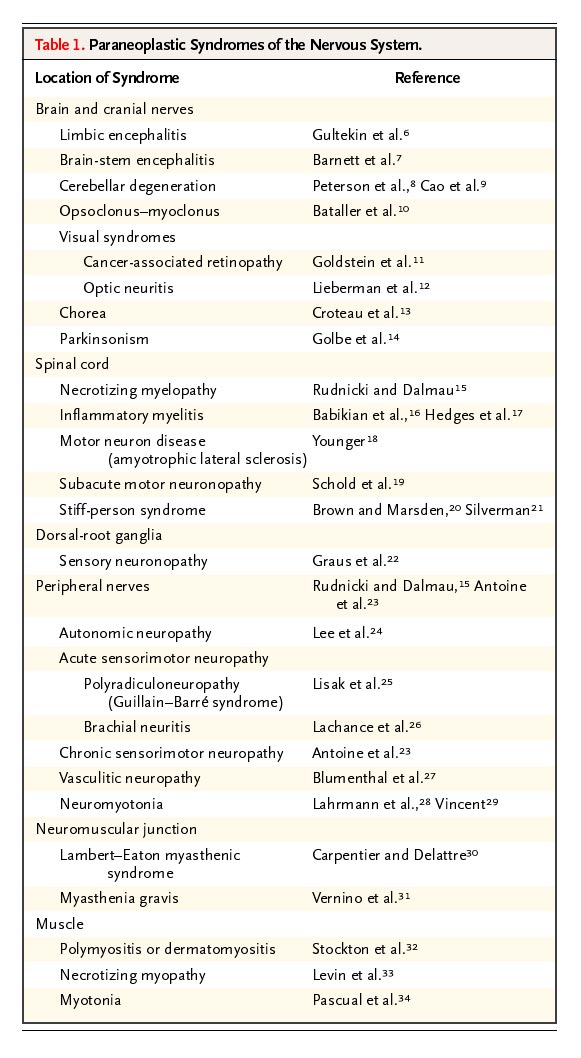

6.28.2004
Color Your Way to 5 A Day
More Color More Health
Growing up you may have been told to eat your greens, but what about your reds, oranges, yellows and blues? The Centers for Disease Control and Prevention and the 5 A Day Partnership encourages YOU to "Sample the Spectrum" of the colorful vegetables and fruit available this season. By putting something of every color on your plate or in your lunch bag, you are more likely to eat the 5 to 9 recommended servings of vegetables and fruit every day. Just think: 1 cup of dark, leafy GREENS, ½ cup of RED tomatoes, ½ cup of YELLOW peppers, 6 oz. ORANGE juice and ½ cup of BLUEberries. And you have 5 A Day! It’s quite simple when you Sample the Spectrum.

The more reds, oranges, greens, yellows, and blues you see on the plate, the more health promoting properties you are also getting from your vegetable and fruit choices. Nutrition research shows that colorful vegetables and fruit contain essential vitamins, minerals, fiber, and phytochemicals that your body needs to promote health and help you feel great. Here are the specifics…
Reds
When you add deep reds or bright pinks to your daily diet, you are also adding a powerful antioxidant called lycopene. Lycopene is found in tomatoes, red and pink grapefruit, watermelon, papaya and guava. Diets rich in lycopene are being studied for their ability to fight heart disease and some cancers.
Greens
Do you know why this color is so essential to your diet? Not only do green vegetables look great and taste wonderful, but they are rich in the phytochemicals that keep you healthy. For example, the carotenoids lutein and zeaxanthin that are found in spinach, collards, kale and broccoli have antioxidant properties and are being studied for their ability to protect your eyes by keeping your retina strong. Also, research is being done on cruciferous vegetables like cabbage, Brussels sprouts, cauliflower, kale, and turnips to see if they may reduce the risk of cancerous tumors! Greens are also loaded with essential vitamins (folate), minerals, and fiber.
Oranges/Yellows
Orange, the color of a blazing sun, is a must have in your daily diet. Orange vegetables and fruits like sweet potatoes, mangos, carrots, and apricots, contain beta-carotene. This carotenoid is a natural antioxidant that is being studied for its role in enhancing the immune system. In addition to being touted as a powerful health-protector, the orange group is rich in Vitamin C. Folate, most often found in leafy greens, is also found in orange fruits and vegetables, and is a B vitamin that may help prevent some birth defects and reduce your risk of heart disease. With a chemical make-up this good, make the orange group always a part of your 5 to 9 a day.
Bright yellows have many of the same perks as the orange groups: high in essential vitamins and carotenoids. Pineapple, for example, is rich with Vitamin C, manganese, and the natural enzyme, bromelain. Additionally, corn and pears are high in fiber. Yellow fruits and vegetables belong to many different families, but they all share the common bond of being health enhancing with great taste. Go for the gold!
Blues/Purples
Blues and purples not only add beautiful shades of tranquility and richness to your plate, they add health-enhancing flavonoids, phytochemicals, and antioxidants. Anthocyanins, a phytochemical, are pigments responsible for the blue color in vegetables and fruits, and are being studied for their role in the body’s defense of harmful carcinogens. Blueberries, in particular, are rich in Vitamin C and folic acid and high in fiber and potassium.
Whites
Vegetables from the onion family, which include garlic, chives, scallions, leeks, and any variety of onion, contain the phytochemical allicin. Research is being conducted on
Allicin to learn how it may help lower cholesterol and blood pressure and increase the body’s ability to fight infections.
Indoles and sulfaforaphanes, phytochemicals in cruciferous vegetables like cauliflower, for how they may inhibit cancer growth.
Polyphenols, another important phytochemical in pears and green grapes for how they may reduce the risk of certain cancers.
Savor the Spectrum All Year Long
There is color in every season. When it comes to your health, you’ll fare best with a multi-colored diet. By putting something of every color on your plate or in your lunch bag, you are more likely to eat the recommended 5 to 9 servings of vegetables and fruits every day. Think color: 1 cup of dark, leafy salad GREENS with WHITE onions sprinkled on top, ½ cup of RED tomatoes, ½ cup of YELLOW pineapple chunks, 6 oz. ORANGE juice and ½ cup of BLUEberries. Delicious and healthy!
Get your "5 to 9 A Day" the Colorful Healthy Way!
'Best Antioxidants List'
MONDAY, June 28 (HealthDayNews) -- A variety of veggies, fruits and nuts battled it out this month for the top spot on a new list of the 20 most antioxidant-rich foods, ranked by nutrition scientists at the U.S. Department of Agriculture (news - web sites) (USDA).
In the end, small red beans won the day, narrowly beating out wild blueberries as the food with the highest concentration of disease-fighting compounds per serving.
Antioxidants fight damage to cells from rogue molecules called "free radicals." Experts believe this assault on cells may fuel killer diseases such as heart disease and cancer, and even aging itself.
The new Top 20 list, published in the June issue of the Journal of Agricultural and Food Chemistry, "is a relative ranking of the capacity of foods to interfere with or prevent oxidative processes and to scavenge free radicals," explained list co-creator Ronald L. Prior, a USDA nutritionist and research chemist based in Little Rock, Ark.
Their Top 20:
1 Small red beans (dried).
2 Wild blueberries.
3 Red Kidney beans.
4 Pinto beans.
5 Blueberries (cultivated).
6 Cranberries.
7 Artichokes (cooked).
8 Blackberries.
9 Prunes.
10 Raspberries.
11 Strawberries.
12 Red Delicious apples.
13 Granny Smith apples.
14 Pecans.
15 Sweet cherries.
16 Black plums.
17 Russet potatoes (cooked).
18 Black beans (dried).
19 Plums.
20 Gala apples.
6.25.2004
Create Pockets to Protect Your Assets
By: Lee R. Phillips
Asset protection is something that you should be concerned about. There are a lot of little things you can do to protect yourself, and, in many cases, the little things add up to create a fairly good asset protection plan.
You can compare protecting your assets to protecting your money from a pickpocket. If all of your money is in your wallet, then you will lose everything if someone steals it. If you take the majority of your money out of your wallet, put some of it in your front pocket, some of it in your money belt, and give some of it to your spouse, then when your wallet is stolen, you won’t lose everything.
When you get sued or attacked financially, if all of your assets are held in the same pot, then they are all subject to loss. If you have put some of the assets in your spouse’s name and some in a family limited partnership (FLP) or limited liability company (LLC), then everything isn’t exposed when the attack comes.
Smart Separation
A major part of asset protection is a division between spouses. My wife and I haven’t owned anything together for decades. I don’t own the house; she does. She owns the land, big savings accounts, stocks, bonds, and all of the assets that aren’t likely to get us in trouble. My legal practice is what may get us in trouble. I own the practice. My wife isn’t my vice president, secretary, or any other type of corporate officer—she has nothing to do with it. As a result, I can’t be sued in my practice and lose the house. I could lose everything I own, but the house isn’t mine. My wife paid for it, and it’s hers.
If the spouse doesn’t work, the breadwinner should give the spouse an allowance each month as a “wage.” Obviously, the allowance isn’t reported for tax purposes, but it is deposited into the spouse’s checking account, which the breadwinner doesn’t sign on; it’s the spouse’s to make house payments, buy clothes, or use in any way he/she wants.
The courts have said that in this strategy the house clearly is the spouse’s, and the argument can’t be made that the breadwinner paid for and owns the house. I own the practice, the rental units, the extra cars, and the other assets that could get us sued. She owns the car she drives, and I own the car I drive because in a lawsuit over a car accident, the owner and the driver usually are sued.
Pocket Concept
The bottom line is that we own nothing in common, and we stack the passive assets behind her and the risky assets behind me. We don’t move assets back and forth between us. We have two clearly defined pockets, and if one of them is emptied, the other one probably will be left alone.
The division of assets can be done easily using each spouse’s name. We use a living revocable trust for each spouse. The trusts don’t give us any more protection, but they solve problems if one of us were to become disabled or die.
If you have significant life insurance, the next pocket to create is an irrevocable life insurance trust (ILIT). This trust is different from the living revocable trust, and it effectively protects the face value and cash value of your life insurance from lawsuits and income and estate taxes. However, you do lose the ability to directly borrow against the cash value.
The next pocket is either the FLP or LLC. They allow you to put assets into the pocket and divide them up with your children, grandchildren, and others. They are simple, and they let you maintain control of the assets, although the ownership of the FLP or LLC is divided up.
Understanding the concept of pockets and how most asset protection techniques rely on using spouses to create or control the pockets should make asset protection clearer. You also should realize that if you can create one clear pocket each for you and your spouse, you have done more to protect your assets than most people ever manage to accomplish.
6.21.2004
Sleep ClassificationThe original diagnostic classification of sleep and arousal disorders
by the Association of Sleep Disorder Centers categorized sleep-wake
disorders into four classes: (1) disorders of initiating and
maintaining sleep, (2) disorders of excessive somnolence, (3)
disorders of sleep-wake schedule, and (4) dysfunctions associated with
sleep, sleep stages, or partial arousals (parasomnias). This
classification has been supplanted by the 1990 International
Classification of Sleep Disorders (ICSD), which was revised slightly
in 1997. The ICSD system is the one used by sleep specialists; it
lists 84 sleep disorders in four broad categories: dyssomnias,
parasomnias, sleep disorders associated with medical or psychiatric
disorders, and proposed sleep disorders
Dyssomniasare subdivided into intrinsic, extrinsic, and circadian rhythm sleep
disorders. Intrinsic disorders result from causes in the body, whereas
extrinsic disorders are primarily caused by environmental factors.
Circadian rhythm disorders result from disruption of sleep-wake
schedule changes.
Parasomnias are characterized by abnormal movements
and behavior intruding into sleep without necessarily disturbing sleep
architecture. These consist of arousal and sleep-wake transition
disorders, REM-related parasomnias, and others.
Medical or psychiatric sleep disorders include those
attributable to another condition; they are caused by mental
(psychiatric), neurological, and other medical disorders.
Proposed sleep disorders include disorders for which
inadequate or insufficient information is available to substantiate
with certainty the existence of that particular disorder.
The ICSD includes descriptive details, specific diagnostic criteria,
severity, and duration. There is also coding information for clinical
and research purposes.
In addition to the ICSD two other systems are used: the International
Classification of Diseases (ICD), ninth revision, clinical
modification, and the ICD, tenth revision (ICD-10). The ICD-10NA is an
expansion of ICD-10 with alphanumeric codes for every neurological
disease, including specific sleep disorders. There has been no study
to assess the validity and reliability of any classification of sleep
disorders.
6.18.2004
Sleep Classification
The original diagnostic classification of sleep and arousal disorders by the Association of Sleep Disorder Centers categorized sleep-wake disorders into four classes: (1) disorders of initiating and maintaining sleep, (2) disorders of excessive somnolence, (3) disorders of sleep-wake schedule, and (4) dysfunctions associated with sleep, sleep stages, or partial arousals (parasomnias). This classification has been supplanted by the 1990 International Classification of Sleep Disorders (ICSD), which was revised slightly in 1997. The ICSD system is the one used by sleep specialists; it lists 84 sleep disorders in four broad categories: dyssomnias, parasomnias, sleep disorders associated with medical or psychiatric disorders, and proposed sleep disorders.
Dyssomnias are subdivided into intrinsic, extrinsic, and circadian rhythm sleep disorders. Intrinsic disorders result from causes in the body, whereas extrinsic disorders are primarily caused by environmental factors. Circadian rhythm disorders result from disruption of sleep-wake schedule changes.
Parasomnias are characterized by abnormal movements and behavior intruding into sleep without necessarily disturbing sleep architecture. These consist of arousal and sleep-wake transition disorders, REM-related parasomnias, and others.
Medical or psychiatric sleep disorders include those attributable to another condition; they are caused by mental (psychiatric), neurological, and other medical disorders.
Proposed sleep disorders include disorders for which inadequate or insufficient information is available to substantiate with certainty the existence of that particular disorder.
The ICSD includes descriptive details, specific diagnostic criteria, severity, and duration. There is also coding information for clinical and research purposes.
In addition to the ICSD two other systems are used: the International Classification of Diseases (ICD), ninth revision, clinical modification, and the ICD, tenth revision (ICD-10). The ICD-10NA is an expansion of ICD-10 with alphanumeric codes for every neurological disease, including specific sleep disorders. There has been no study to assess the validity and reliability of any classification of sleep disorders.
Stanford sleepiness scale
Wide awake, active, and alert
Awake and able to concentrate but not functioning at peak
Relaxed, awake, and responsive but not fully alert
Feeling a little foggy
Difficulty staying awake
Sleepy, prefer to lie down
Cannot stay awake; sleep onset is imminent
Source: Modified with permission from Hoddes, E., Zarcone, V., Smythe, H., et al. 1973, "Quantification of sleepiness: A new approach," Psychophysiology, vol. 10, pp. 431-436.
Epworth sleepiness scale
Eight situations Scores*
1. Sitting and reading -
2. Watching television -
3. Sitting in a public place (e.g., a theater or a meeting) -
4. Sitting in car as a passenger for an hour without a break -
5. Lying down to rest in the afternoon -
6. Sitting and talking to someone -
7. Sitting quietly after a lunch without alcohol -
8. In a car, while stopped for a few minutes in traffic -
*Scale to determine the total scores: 0 = would never doze; 1 = slight chance of dozing; 2 = moderate chance of dozing; 3 = high chance of dozing.
Source: Modified with permission from Johns, M. W. 1991, "A new method for measuring daytime sleepiness: The Epworth sleepiness scale," Sleep, vol. 14, pp. 540-545.
Causes of transient and short-term insomnia
A change of sleeping environment (the most common cause of transient insomnia, the so-called first night effect)
Jet lag
Unpleasant room temperature
Stressful life events (e.g., loss of a loved one, divorce, loss of employment, preparing to take an examination)
Acute medical or surgical illnesses (including intensive care units)
Stimulant medications (e.g., theophylline, beta blockers, corticosteroids, thyroxine, bronchodilators, or withdrawal of central nervous system depressant medications)
Jet lag is experienced after travel through several time zones, which disrupts the synchronization between the body's inner clock and external cues (Bearpark 1994). Some of these sleep problems result from "jet" factors and others from "lag" factors. Jet factors that may be detrimental to sleep include long periods of travel with limited mobility, dryness of the eyes, headache, fatigue, gastrointestinal disturbances, and nasal congestion. Lag factors result in dyssynchrony between the body's internal clock and the sleep schedule of the new environment. Symptoms are usually most pronounced when travel is from west to east and are more severe in elderly individuals. Readjustment and resynchronization occur at a rate of about 1 hour per day when one travels eastward and 1.5 hours per day when one travels westward (Bearpark 1994).
Shift work may affect up to 5 million workers in the United States; it can cause sleep disruption, chronic fatigue, gastrointestinal symptoms (including peptic ulcer), an increased chance of traffic accidents, and increased errors on the job. Drug-related insomnia includes rebound insomnia on discontinuation of short- and intermediate-acting hypnotics.
6.17.2004
Primary headache associated with sexual activity
By: Hamid R Sami and James R Couch
ICD Code 784.0
Synonyms Benign coital cephalgia; Coital headache; Orgasmic cephalgia; Sexual headache, Benign sex headache
Historical note and nomenclature
Headache related to sexual activity has been recognized since the time of Hippocrates, who first suggested that headache might be brought on by "immoderate venery." In modern times, headache has provided subject matter for comedians and is usually relegated to a stereotype of avoidance of sexual activity on the part of the female (“Not tonight dear, I have a headache”). In fact, headache may be caused, exacerbated, or relieved by sexual activity. Wolff was the first to recognize that a benign headache syndrome could arise in association with sexual activity (Wolff 1963). The condition has been given a number of names including "orgasmic cephalgia," "benign coital cephalgia," "coital headache," or "headache associated with sexual activity" (Martin 1973; Paulson and Klawans 1974; Headache Classification Committee of the International Headache Society 1988; Couch 1993).
The relationship between headache and sexual activity can be categorized as follows:
A. Headache specifically related to sexual activity
B. Exacerbation of current headache
C. Headache relief with sex (Couch and Bearss 1990; Evans and Couch 2001)
A. New Onset Headache Specifically Related to the Sexual Activity
1. Primary Headache=Benign Coital Cephalgia
2. Secondary Headache
a. Subarachnoid hemorrhage (gross hemorrhage or leak), related to aneurysm, arteriovenous malformation or angioma rupturing during sexual activity
b. Headache due to distension of aneurysm
c. Headache with carotid or vertebral dissection
d. Headache associated with stroke during sex
e. Headache due to CNS vasculitis related to amine-related drugs (amphetamine, cocaine) taken as “recreational” drugs
f. Headache due to drugs taken specifically to enhance sexual pleasure
g. Headache due to increased intracranial pressure related to physical activity due to sex. This is most important in subjects with pre-existing condition such as Arnold-Chiari malformation or space-occupying lesion
h. Headache related to muscle tension, muscle rupture, or fascial tear in neck related to sexual activity
i. Low CSF pressure headaches due to dural leak
Clinical manifestations
Sexual intercourse and climax may be associated with marked increase in heart rate and blood pressure, which may cause headache directly or indirectly. In addition, headaches may occur during sexual activities associated with intercourse or independent of intercourse (eg, masturbation), or orgasm. Men are affected much more often than women (4:1 ratio), which may, in some circumstances, relate to the degree of physical exertion in the sexual act. The age at onset ranges from the second through the sixth decades of life, with a mean age of 40 years (Braun and Klawans 1986).
Forty percent of patients with sexual headaches also experience benign exertional headache (Silbert et al 1991). A personal or family history of migraine is common but not absolute (Lance 1976; Silbert et al 1991; Ostergaard and Kraft 1992). Headaches are more frequent during attempts to have several orgasms during one sexual encounter.
Benign headaches or benign coital cephalgia associated with sexual activity can be divided into three types:
(1) Preorgasmic tension-type headache. A dull, tight, cramping headache, usually bilateral and occipital/cervical in location, can occur during sexual activity. It usually intensifies as sexual excitement increases and is generally preorgasmic. The headache is similar in quality to tension-type headache. It may be related to excessive contraction of head and neck musculature and is believed to arise in association with the spasm of craniofacial and cervical musculature that occurs prior to orgasm (Lance 1974; 1976).
(2) Orgasmic. Headaches with abrupt or explosive onset, in the occipital region, behind the eyes, or generalized, occur at orgasm (Pascual et al 1996). This type of headache builds as the subject approaches orgasm and then “explodes” to a severe, generalized headache with orgasm. The headache can be prevented by not allowing orgasm to occur. Such headaches are usually throbbing, of varying intensity, and rather short-lived with a duration of minutes to a few hours. They are the most common type associated with sexual activity (Johs 1986; Ostergaard and Kraft 1992). While the etiology is unknown, it has been postulated to be caused by the increased blood pressure that occurs during orgasm (Lance 1974; 1976). As the headache may outlast the elevation of blood pressure that occurs with sexual activity, this appears to be an incomplete or inadequate pathophysiologic mechanism. This type of headache appears to share clinical features with migraine, and some authors consider it to be a migraine variant (Martin 1973; Lance 1976; Levy 1981; Porter and Jankovic 1981).
(3) Postorgasmic headache upon standing. This headache, a result of low cerebrospinal fluid pressure, can result from a dural tear that occurred during the physiologic stress of coitus. The relationship of posture to pain in these patients is identical to that seen in patients with headache following lumbar puncture.
Recently, a new type of pain triggered by sexual activity has been described (Jacome 1998). Two men (one with compressive cervical myelopathy, the second with a tethered cord and intraspinal lipoma) experienced severe, paroxysmal, icepick-like pains referred to the neck in the first and to the groin and genital area in the second.
The diagnostic criteria for headaches associated with sexual activity published by the International Headache Society are listed in Table 1 (Headache Classification Subcommittee of the International Headache Society Cephalalgia Volume 24 Supplement 1 2004).
Table 1. Diagnostic Criteria for Benign Headache Associated with Sexual Activity or Benign Orgasmic Headache
Description: Headache precipitated by sexual activity, usually starting as a dull bilateral ache as sexual excitement increases and suddenly becoming intense at orgasm, in the absence of any intracranial disorder.
Preorgasmic headache diagnositic criteria:
A. Dull ache in the head and neck associated with awareness of neck and/or jaw muscle contraction and fulfilling criterion B
B. Occurs during sexual activity and increases with sexual excitement.
C. Not attributed to another disorder.
Orgasmic headache diagnositic criteria:
A. Sudden severe (`explosive`) headache fulfilling criterion B
B. Occurs at orgasm
C. Not attributed to another disorder.
Headaches associated with sexual activity appear to have an unpredictable clinical pattern. They may appear suddenly, continue to occur for months to years, and stop abruptly, or they may occur regularly for many years (Johs 1986; Ostergaard and Kraft 1992). The headache may not occur with every attempt at sexual activity or may occur to an extent that proscribes any sexual intercourse.
Most coital headaches are benign, but some are malignant. Thus bleeding associated with subarachnoid hemorrhage may occur at the time of intercourse (Fisher 1968; Lundberg and Osterman 1974). It is estimated that sexual intercourse is the precipitating cause of subarachnoid bleeding in 3.8% to 12% of patients with saccular aneurysms (Locksley 1966; Lundberg and Osterman 1974; Adams et al 1980), and in 4.1% of patients with arteriovenous malformations (Locksley 1966). Vomiting, meningitis, disturbance of consciousness, and residual pain the day after the incident characterize the headache caused by subarachnoid hemorrhage and help to distinguish it from that of benign orgasmic cephalgia. In addition, cases of cerebral or brainstem infarction with headache have been reported (Lance 1976; Levy 1981; Martinez et al 1988). Some of these cases may represent instances of complicated migraine (Levy 1981).
Clinical vignette
Case 1. A 46-year-old male noted the onset of headache with sexual activity for the first time one week earlier. During intercourse, he noted a painful tight sensation in the suboccipital and occipital regions. This pain increased as he neared climax. At orgasm, he experienced an explosive, severe, holocranial headache that was sharp and aching in character. The pain was so severe he immediately ceased any activity and collapsed into the fetal position. This extremely severe pain lasted for 5 to 10 minutes and began to remit slowly. The patient was taken to a local emergency room where there was no meningismus and neurologic examination and CT of head were normal. Several days later the patient again attempted sexual intercourse and noted the same premonitory pain. He stopped the intercourse and the pain did not worsen and then remitted.
Case 2. A 43-year-old female noted the onset of severe bilateral headache during sexual intercourse. It built to a peak of severe headache at orgasm. The headache was not associated with nausea, photophobia, or phonophobia, and would remit within 30 to 60 minutes. The patient subsequently noted that this did not happen every time she had intercourse. If she prevented herself from experiencing orgasm when she experienced the premonitory headache, she could prevent the severe explosive headache from occurring. The patient was treated with indomethacin before intercourse and had partial improvement. The patient was followed for two years and the intercourse-related headache remitted after the first year.
Case 3. A 41-year-old woman was seen with a 20-year history of headache. The headaches were associated with nausea and light and noise sensitivity. For about 5 years, 90% of the time when she had an orgasm, she would immediately develop a typical headache without aura which could last up to 3 days. Neurologic examination was normal, as was MRI of the head. A diagnosis of migraine with benign coital cephalgia was made.
The prevalence of orgasmic headache is not known exactly (Evans and Couch 2001), but there are some reports with prevalence of 0.21% to 1.3% (Akpunonu and Ahrens 1991). Many patients with sexual headache have a background of migraine. Most patients who reported headache with orgasm or with proximity to orgasm often find that there is no headache or only mild headache if sexual activity is not allowed to proceed to orgasm.
Etiology
Benign headaches related to sexual activity can be caused by excessive cervical and facial muscular contraction, a dural tear, or increased blood pressure. Lance has postulated a period of muscular contraction during the short period preceding climax and a vascular component related to hypertension at the time of climax (Lance 1974; 1976). Segmental vasospasm of cerebral arteries was documented by magnetic resonance imaging or digital angiography before, during, and after resolution of the orgasmic headache. (Valenca and Valenca et al. 2004)
Risk factors associated with sexual headaches include: hypertension, obesity, lack of exercise, psychosexual stress (including extramarital affairs), the degree of sexual excitement, kneeling position during sexual intercourse, history of migraine or exertional headache, family history of headache and occlusive arterial disease (Paulson 1975; Kraft 1979; Mann et al 1982; Akpunonu and Ahrens 1991).
Exertion and sexual activity can also produce headaches in patients who have mass lesions, structural malformations (eg, Chiari malformation), and vascular malformations. Bleeding from an aneurysm or arteriovenous malformation can cause headaches associated with sexual activity.
At least one report has described the familial occurrence of vascular sexual headache (Johs 1986).
Coital headache may arise as a side effect of sexual stimulants such as amyl nitrite, marijuana, amphetamines and some commonly used anxiolytics as well as Sildenafil (Goldstein 2001). In meta-analysis of Sildenafil for male erectile dysfunction, headache was reported in 11% of patients (Fink et al 2002).
Pathogenesis and pathophysiology
According to Masters and Johnson, the basic physiologic response of both men and women to sexual stimulation is diffuse vasodilation followed by a secondary generalized increase in muscle tension (Masters and Johnson 1966). In particular, the neck and face muscles involuntarily contract. Elevations of blood pressure (as much as 50 mm Hg diastolic and 100 mm Hg systolic in men) are found at the time of orgasm (Littler et al 1974; Nemac et al 1976). The acute pressor response is comparable to the paroxysmal elevations in blood caused by pheochromocytomas. The headaches in both conditions resemble each other. It is unclear if the orgasmic headache is related to the increase in blood pressure, cerebral vasodilation, or other factors such as increase in neural activity and/or release of neurotransmitters.
Epidemiology
Rasmussen and Olesen have assessed the lifetime prevalences of headache disorders in a cross-sectional epidemiologic survey of a representative 25- to 64-year-old general population (Rasmussen and Olesen 1992). They found a lifetime prevalence of 1% for orgasmic headache. Others reported a prevalence of 0.21% to 1.3% (Akpunonu and Ahrens 1991).
Prevention
Headaches may be prevented in some patients by weight loss, an exercise program, a more passive role during intercourse, variation in positions, limitation of sexual activity during a given day, and drug therapy.
Differential diagnosis
The alert clinician must be aware that a severe and disabling headache at the time of intercourse may result from subarachnoid bleeding as the result of rupture of a saccular aneurysm, or AVM. Other considerations include carotid/vertebral dissection as well as stroke. The subsequent course of the headache should differentiate the benign from the malignant forms of head pain. Whether stretching of an aneurysm without rupture may produce a headache has never been proven.
Diagnostic workup
A careful history and physical examination are essential. All patients seen acutely and suspected of having a subarachnoid hemorrhage should have a CT scan and a lumbar puncture. Patients with chronic sexual headaches should have an MRI examination.
Prognosis and complications
The prognosis for recovery is excellent.
Management
The therapy of headaches associated with sexual activity is difficult to evaluate because of the capricious nature of the disorder. Treatment approaches are either nonpharmacological, such as abstinence, a passive role during intercourse, varying positions during sexual activities, weight reduction, increased exercise, biofeedback and relaxation therapy; or pharmacological, such as analgesics, antihistamines, antidepressants, as well as beta blockers and calcium channel blockers (Akpunonu and Ahrens 1991). For sex-induced vascular headaches that are severe and occur regularly, treatment with Inderal (40 mg to 240 mg a day) or other beta blockers has been successfully used in some patients (Porter and Jankovic 1981). Indomethacin (25 mg/day to 75 mg/day on a regular or intermittent basis) has also been recommended (Diamond and Dalessio 1982). No drug therapy has been successful in 100% of cases.
B. Exacerbation of current headache
An association between primary headache associated with sexual activity and migraine is reported in approximately 50% of cases (IHS report in Cephaalgia 2004).
Many migraineurs report worsening of their headache intensity or frequency during and after sexual activities. In 51 patients with the diagnosis of Headache associated with sexual activity (HAS), there was a high comorbidity with migraine (25%), benign exertional headache (29%), and tension-type headache (45%). (Ferese et al 2003)
C. Relief of migraine by sexual activity
Headache relief with sex. The major emphasis of material on sex and headache has related to causation or exacerbation of headache with sexual activity. Couch and colleagues (Couch and Bearss1990; Evans and Couch 2001) reported on relief of migraine with sexual intercourse. A group of 82 women being screened for participation in a study of Fiorinal and headache were asked whether they had had sexual intercourse during their migraine. Of 57 who reported they had, 27 noted significant headache relief with sexual intercourse. Of these, 10 noted that orgasm produced complete remission of the migraine without recurrence and four noted more than 50% improvement. The remainder noted temporary relief of approximately an hour, or only modest relief. Of note, triptans typically provide complete relief or “pain free” state in 27% to 33% of subjects (Ferrari 2001).
Consequently, sexual activity with orgasm may actually be therapeutic in a significant minority of women. Men have not been tested.
Pregnancy
An unusual case of acute headache and hypertension occurring at the height of sexual excitement during the puerperium has been reported. Further information is not available at this time.
Anesthesia
This diagnosis does not preclude anesthesia as indicated or necessary.
References
Adams HP, Jergenson DD, Kassell NF, Sahs AL. Pitfalls in the recognition of subarachnoid hemorrhage. JAMA 1980;244:794-6.
Adinma JI. Acute puerperal coital headache and hypertension. Aust N Z J Obstet Gynaecol. 1994 Aug;34(4):487-8
Akpunonu BE, Ahrens J. Sexual Headaches: case report, review, and treatment with calcium blocker. Headache 1991;31(3):141-5.
Braun A, Klawans H. Headaches associated with exercise and sexual activity. In: Handbook of Clinical Neurology. Rose FC, editor. Amsterdam: Elsevier Science Publishers, 1986:373-82.
Couch JR. Headache to worry about. Med Clin North Am 1993;77(1):141-67.
Couch JR, Bearss C. Relief of migraine with sexual intercourse. Headache 1990;30:302.
Diamond S, Dalessio DJ. The practicing physician's approach to headache. 3rd ed. Baltimore: Williams & Wilkins, 1982:72-3.
Evans RW, Couch JR. Orgasm and migraine. Headache 2001;41(5):512-4.
Ferrari MD, Roon KI, Lipton RB, Goadsby PJ. Oral triptans (serotonin 5-HT (1B/1D) agonists) in acute migraine treatment: a meta-analysis of 53 trials. Lancet 2001;358(9294):1668-75.
Fink HA, Mac Donald R, Rutks IR, Nelson DB, Wilt TJ. Sildenafil for male erectile dysfunction: a systematic review and meta-analysis. Arch Intern Med 2002;162(12):1349-60.
Fisher M. Headaches in cerebral vascular disease. In: Vinken PJ, Bruyn GW, editors. Handbook of clinical neurology. Vol. 5. Amsterdam: North Holland Pr, 1968:124-56.
Frese A, Eikermann A, Frese K, Schwaag S, Husstedt IW, Evers S. Headache associated with sexual activity: demography, clinical features, and comorbidity. Neurology. 2003 Sep 23;61(6):796-800
Goldstein J. Sexual aspects of headache. How sexual function relates to headaches and their causes and treatment. Postgrad Med 2001;109(1):81-4, 87-8, 92.
Headache Classification Committee of the International Headache Society. Classification and diagnostic criteria for headache disorders, cranial neuralgias and facial pain. Cephalalgia 1988;8(Suppl 7):1-96.
Jacome DE. Masturbatory-orgasmic extracephalic pain. Headache 1998;38:138-41.
Johs DR. Benign sexual headache within a family. Arch Neurol 1986;43:1158-60.
Kraft M. Benign coital cephalgia. Ugeskr Laeger 1979;141:2454-5.
Lance JW. Headaches occurring during sexual intercourse. Proc Aust Assoc Neurol 1974;11:57-60.
Lance JW. Headaches related to sexual activity. J Neurol Neurosurg Psychiatry 1976;39:1226-30.
Levy DK. Stroke and orgasmic cephalgia. Headache 1981;21:12-4.
Littler WA, Honour AJ, Sleight P. Direct arterial pressure, heart rate and electrocardiogram during human coitus. J Reprod Fertil 1974;40(2):321-31.
Locksley HB. Natural history of subarachnoid hemorrhage, intracranial aneurysms and arteriovenous malfunctions: based on 6368 cases in the cooperative study. J Neurosurg 1966;25:219-39.
Lundberg PD, Osterman P. The benign and malignant forms of orgasmic headache. Headache 1974;14:164.
Mann S, Miller Craig MW, Gould BA, Melville DI, Raftery EB. Coital blood pressures in hypertensives, cephalgia, syncope, and the effects of beta-blockade. Br Heart J 1982;47:84-9.
Martin EA. Severe headache accompanying orgasm. Br Med J 1973;4:44.
Martinez JM, Roig C, Arboix A. Complicated coital cephalgia. Three cases with benign evolution. Cephalalgia 1988;8:265-8.
Masters WH, Johnson VE. Human sexual response. Boston: Little Brown, 1966.
Nemac ED, Mansfield L, Kennedy JW. Heart rate and blood pressure responses during sexual activity in normal males. Am Heart J 1976;92:274-7.
Ostergaard JR, Kraft M. Benign coital headache. Cephalalgia 1992;12:353-5.
Pascual J, Iglesias F, Oterino A, Vázquez-Barquero A, Berciano J. Cough, exertional, and sexual headaches: an analysis of 72 benign and symptomatic cases. Neurology 1996;46:1520-4.
Paulson GW. Headaches associated with orgasm. Med Aspects Hum Sex 1975;9:7-16.
Paulson GW, Klawans HL. Benign orgasmic headache. Headache 1974;13:181.
Porter M, Jankovic J. Benign coital cephalgia. Differential diagnosis and treatment. Arch Neurol 1981;38:710-2.
Rasmussen BK, Olesen J. Symptomatic and nonsymptomatic headaches in a general population. Neurology 1992;42:1225-31.
Silbert PL, Edis RH, Stewart-Wynee EG, Gubbay EG. Benign vascular sexual headache and exertional headache: interrelationships and long term prognosis. J Neurol Neurosurg Psychiatry 1991;54:417-21.
Valenca MM, Valenca LP, Bordini CA, da Silva WF, Leite JP, Antunes-Rodrigues J, Speciali JG. Cerebral vasospasm and headache during sexual intercourse and masturbatory orgasms. Headache. 2004 Mar;44(3):244-8.
Wolff HG: Headache and Other Head Pain. New York: Oxford University Press, 1963.
CPRmaker
- A freeware application based on powerful Filemaker database that specifically designed for neurologists and is customized to run on PC or Mac.
- It can be run from any storage device such as USB drives for ultimate mobility and ease of access and recording.
- Customizable interface for your practice name, address, logo etc.
- Can be used with any speech recognition softwares for saving you dictation costs.
- Small size, only 5 megabyte, A very simplified software for non-savvy computer users.
- The version 2 has interfaces for EEG, EEG report, EMG, EMG report as well as normal values for EMG based on Preston EMG book.
Click on the link to download my software: Window
CPRmaker Mac
CPRmaker
6.13.2004
6.04.2004
6.03.2004
AIDS CNS- d/t HIV, Opportunistic infections, Neoplasm
In HIV pt the most common brain lesions- toxo, B cell NHL, pyogenic abcess, syphylis, PML, mets
Tx of toxo- pyrimethamine and sulfadiazine are of initial benefit in up to 90% of patients. most adult in US have ab indicative of prior exposure. Cerebral involvement is thought to represent reactivation of a late primary infection.
AIDS dementia- subcortical, PM slow, impaired concentration, reading and forgetfulness"
1.10.2004
Patient Condition and Choice of Antihypertensive Drugs
Conditions
Drug Choice
No comorbid conditions
Diuretics
Isolated systolic hypertension (elderly patients)
Diuretics (preferred), calcium antagonists (DHP)*
Angina
Beta blockers,* calcium antagonists (non-short-acting DHP)
Angina (with diabetes or LV dysfunction)
ACE inhibitors† (in addition to beta blockers and calcium antagonists)
Atrial fibrillation
Beta blockers,* calcium antagonists (rate limiting)*†
Cough with ACE inhibitors
ARBs*
Diabetes mellitus type 1 with proteinuria
ACE inhibitors*; calcium antagonists (non-DHP); diuretics, beta blockers†
Diabetes mellitus type 2 with proteinuria
ARBs*†; calcium antagonists (non-DHP)†; diuretics, beta blockers†
High risk of type 2 diabetes
ACE inhibitors†
Essential tremor
Beta blockers (noncardioselective)†
Heart failure, LV dysfunction
ACE inhibitors, beta blockers, diuretics, aldosterone antagonists*; ARBs†; generally, an ACE inhibitor is first choice, ± a beta blocker in asymptomatic patients; diuretic used to treat congestion; aldosterone antagonist used only in advanced disease in combination with other agents; ARB should not be used in patients on an ACE inhibitor and beta blocker [see 1:II Heart Failure]
High risk of cardiovascular disease or type 2 diabetes
ACE inhibitor†
Hyperlipidemia
Alpha blockers (not considered first-line therapy)†
Intolerance to other antihypertensive drugs
ARBs†
Left ventricular hypertrophy (by ECG)
ARBs†
Migraine
Beta blockers (noncardioselective), calcium antagonists (non-DHP)†
Myocardial infarction
Beta blocker (non-ISA) most often drug of choice, with ACE inhibitor added if LV function impaired*; aldosterone antagonist can be added to standard therapy in patients with LV dysfunction*; diltiazem (non-Q wave infarction)†; verapamil†
Osteoporosis
Thiazide diuretics†
Peripheral vascular disease
Calcium antagonists†
Preoperative hypertension if at increased cardiovascular risk
Beta blockers†
Previous stroke
Diuretic + ACE inhibitor*; ACE inhibitor as monotherapy had no effect on BP or outcome; benefit noted only with combination that lowered BP
Prostatism
Alpha blockers (not considered first-line therapy)†
Renal insufficiency with proteinuria from any cause
ACE inhibitors, ARBs, calcium antagonists (non-DHP)†
*Compelling indication.
†Specific indication.
ACE—angiotensin-converting enzyme ARB—angiotension II receptor blocker DHP—dihydropyridine ISA—intrinsic sympathomimetic activity LV—left ventricle
Contraindications to Antihypertensive Drugs
Class of Drug
Possible Contraindications
Compelling Contraindications
Diuretics
Dyslipidemia (high doses), allergy to sulfa-based antibiotics, patient is sexually active man, diabetes mellitus (high doses)
Gout, allergy to sulfa-based diuretics
Beta blockers
Bronchospastic disease (asthma, COPD, noncardioselective agents), dyslipidemia (non-ISA agents), severe peripheral vascular disease, athletes
Bronchospastic disease (noncardioselective agents) second- or third-degree heart block
ACE inhibitors, ARBs
Renovascular disease (bilateral renal artery stenosis), renal insufficiency
Pregnancy, hyperkalemia
Calcium antagonists
—
Second- or third-degree heart block (non-DHP agents); heart failure (except amlodipine, felodipine)
Alpha blockers
Postural hypotension
Urinary incontinence
Reserpine
Peptic ulcer, nasal allergy
Depression
Methlydopa
Liver disease
—
Labetalol
Liver disease
—
Central alpha agonists
Depression, sleep disorders
—
ACE—angiotensin-converting enzyme ARBs—angiotensin receptor blockers COPD—chronic obstructive pulmonary disease DHP—dihydropyridine ISA—intrinsic sympathomimetic activity
Archives































